KOH test to diagnose fungal presence in skin and nails is usually done in cases where the patient has an itchy, rash, or scaly skin that is suspected to be caused by the fungus.
How is this test done? Is there anything that needs to be considered before the test? If you are concerned about this issue, please read the useful information as follows.
Understand About Mycology
Fungi is a damaged skin condition caused by a fungal agent. The disease can appear in many different places on the body. In particular, dermatophytes often cause damaged skin, concentrated in places with keratin, also known as keratin such as skin, hair, and nails.
Mycology will cause itching, discomfort, inconvenience, and affect the daily activities of the patient.
Common types of skin fungus can be:
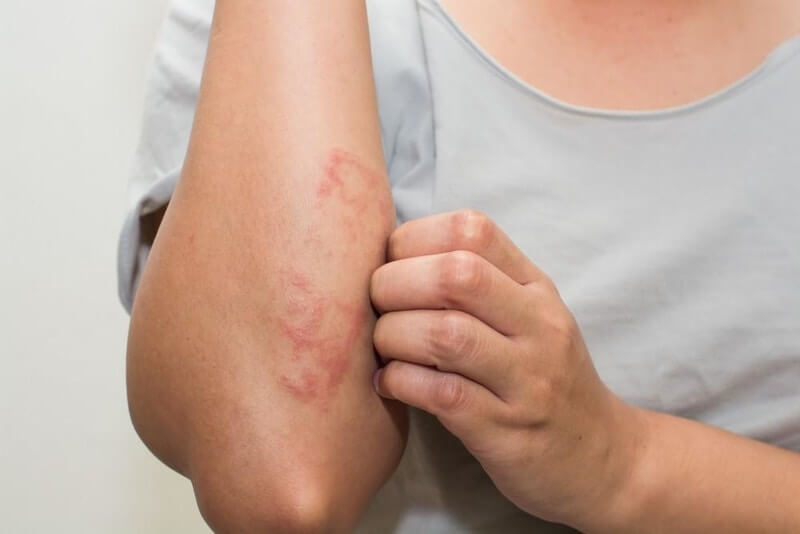
Ringworm: When you have ringworm, it causes an itchy sensation at first, then in the damaged skin will appear a red streak, with a border, observing a clear border, especially on this border has dotted blisters. When the sick person scratches, blisters burst and can spread to different areas of the body.
Ringworm can also spread to healthy people by sharing living utensils with sick people such as towels, clothes, or when sharing beds …
Vitiligo: Ringing is a condition caused by the fungus pityrosporum. It is divided into two types: white langur and black langur.
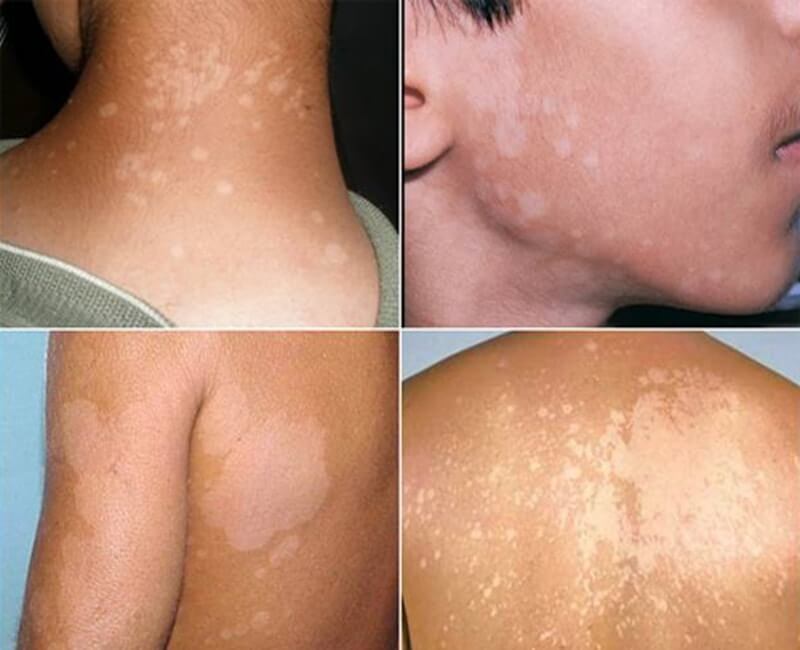
When infected, it will cause an uncomfortable itchy sensation, especially when the patient sweats a lot or goes out in the sun. The risk of getting vitiligo depends on the patient's resistance, skin hygiene, and skin pH and humidity.
Onychomycosis: Candida albicans, trichophyton are usually the typical cause of onychomycosis.
The characteristic manifestations of the disease are nails that are missing or protruding, nails have lost their natural gloss, on the surface of the nail with holes or grooves, it will become increasingly rough and turn yellow. Occasionally swollen and pus develops in the skin at the corner of the nail.
Interstitial fungi: The fungus candida Albicans, epidermophyton, trichophyton fungus are the main causes of interstitial fungal disease. The disease is common in people who regularly soak their feet underwater for many hours such as farmers, swimmers, cleaning workers …
Hair fungus: The fungus piedra shortage is the main cause of hair fungus, with signs that each strand of hair will have many black particles attached to the hair shaft.
In the case of hair fungus caused by trichophyton fungus, it will be accompanied by a damaged scalp manifestation with many small round marks ranging in size from 3 to 5 mm, itchy scalp, and thin scales on the scalp.

Clinically, depending on the type of fungus that causes disease, the image of the lesion is different. Although the disease does not cause serious pain, it affects many daily activities, so it should be diagnosed and treated early.
Usually, when a person is suspected of having fungal skin or nail fungus, the doctor will ask the patient to perform a fungal skin test. In particular, the test commonly used is fresh screening KOH to diagnose mycology (directly under a microscope) or can be cultured in a suitable environment to help doctors identify the fungus causing the disease.
Method of KOH Direct Exam
What is the mycology direct exam for? Most of the time, when looking at the fungal skin condition found in the male genital area or other locations, if you look at the appearance, the doctor cannot accurately diagnose the skin fungus. But through the fresh test, KOH will be a popular method to accurately determine the status of fungal skin and onychomycosis in patients.
To perform a KOH direct exam, the doctor will use a medical instrument to take tissue samples in the area suspected of being smeared with KOH and then fake keratin by heating to remove the main component of the skin. Then, the doctor observes the tissue sample under a microscope to determine the composition of the fungus.
Mycology presence in nail and hair with KOH is usually indicated in the following cases:
• When red, itchy patches of skin appear, look for a scaly and raised border that resembles bullae.
• Nails are brittle, very brittle and thickened, and deformed abnormally.
• Vaginal itching, discomfort, and discharge.
• White patches on the inside of the mouth appear.
How Is KOH Direct Exam Done?

Prepare
To take a sample for the test, a doctor or health professional will need to prepare the necessary equipment including microscope, optical microscope, lamination, sterile scalpel, alcohol lamp, 90-degree alcohol, nail cutting pliers, hair tweezers, and KOH solution at 10-30% concentration.
Patients need to follow the instructions of their doctor to coordinate more smoothly when performing the test. If there are still questions, the patient can consult a doctor for relevant information.
Take sample
For a sampling of skin specimens, follow the steps below:
• Shave the flakes of the skin at the edges of the affected area.
• The doctor can shave in many different positions.
• The shaving method will create from the inside of the damaged area to the outside to remove the skin flakes at the boundary between the diseased skin and normal skin.
• Allow scabs of skin to fall on a prepared specimen or drop into sterile Petri dishes.
• Removes scales that are not sebum.
• The doctor will not scrape samples from acute lesions or superinfection.
For nail specimen collection, the following steps are to be taken:
• In the case of thick nail damage on the free margin, the doctor will use scissors or a knife to scrape and partially cut off the purulent keratin layer underneath the nail.
• In the event of an injury to the nail separating the nail or nail table, the doctor will use a knife with a sharp point to scrape the degenerated substance from the lower part of the nail.
• In the case of inflammation around the nail, the doctor will scrape off a scab located in the furrow around the patient's nail.
• The specimen is the horny layer that will be placed on the specimen or possibly a sterile Petri dish.
Template making
• The examiner will use a reagent to drip 1-2 drops onto the template.
• Cover the green bar.
• Wait for 15 – 30 minutes or if you want to immediately observe this sample over an alcohol lamp flame.
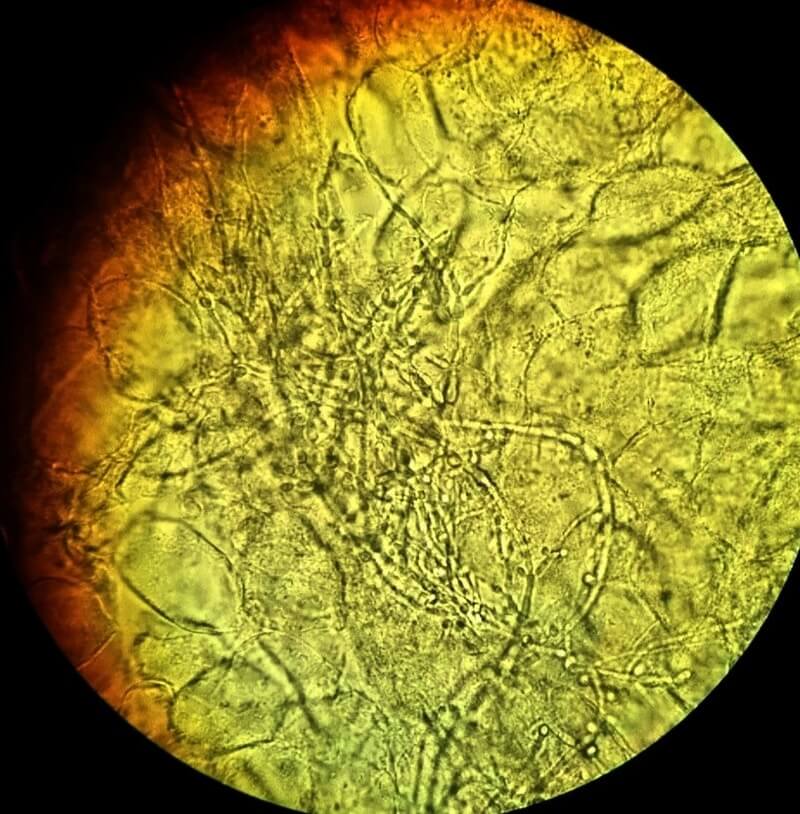
• Next, you will need to thin the template, which is then viewed under 10x and 40x objective microscopes.
• After observing, mycology test results obtained will be recorded on the test sheet and returned to the clinician.
Reading KOH Test Results
Results are normal
For normal results on a fresh scan of KOH, no fungus will be found on the skin. However, if there is doubt, the doctor may need to repeat the test and take multiple samples from different skin areas to confirm the results with certainty.
If the results are still not unusual, the doctor may need to do some more diagnostic tests to find out the cause of the skin damage.

Results are abnormal
There appears fungus in the skin sample undergoing the test.
• Tinea versicolor: Coarse and short mycelium, round cells shaped like a toad's egg sac.
• Tinea pedis: There are transparent fibers, can see spores, and have septum.
• Gray fungus: The mycelium has a septum, divides the bar, and is usually dark in color.
• Hair fungus: Seeing mycelium spores and filaments located in the heart of the hair fibers (internal growth), and the mycelium spores will lie around the hair fibers (emitting).
Test results can also be influenced by the following factors:
Sample samples: In order to have accurate test results, in order to improve treatment results, before conducting the test, patients need to stop antifungal drugs for at least 1-2 weeks. Because if you do not stop the drug, the fungus will temporarily go away or disappear, making it difficult to detect the disease.
The ointments applied during the treatment process that is still present on the skin can make it difficult to observe the specimen, affecting the fresh examination by KOH in the diagnosis of mycology.
The dyes also cause the skin to color, obscuring the structure of the fungus, also hindering the diagnosis of the cause of the disease.
The fungus technician should have professional experience, advanced orientation based on the patient's clinical symptoms informed by the treating doctor in order to improve diagnostic results.
Pay attention to the hygienic conditions of the sampling equipment and the test atmosphere as there are some hyphae and spores commonly present in the air. In the case of not paying attention to clean and clean, it is easy to infect and affect the test results.
In addition to the KOH method to diagnose skin and nail fungus, depending on the case, the doctor can diagnose the disease through the fungus culture test to determine the cause of the disease and combine it with other clinical symptoms.
After the diagnosis confirms the condition, the doctor will prescribe the patient the appropriate antifungal drugs to help bring the most positive treatment effect.
When you have a suspicion of fungal skin disease, want to be consulted before the test, you can also call hotline 19001717 – Diag Medical Diagnostic Center in Ho Chi Minh City for advice and appointment schedule.
Thus, the KOH test for mycology presence in nails and hair has high diagnostic value, helping to make an effective treatment regimen. However, to know the exact condition of the disease, the patient should go to the hospital for consultation and give the most effective method of diagnosis and treatment.
Please find the nearby location or the nearest branch your home to visit for tests and get quick online results. For more detailed information about our test menu and price list, click here.
The site cannot and does not contain medical advice. The medical information is provided for general informational and educational purposes only and is not a substitute for professional advice. Accordingly, before taking any actions based upon such information, we encourage you to consult with the appropriate professionals.

 1900 1717
1900 1717 