Pericoronitis is one of the most common oral diseases, experiencing pain long that affects eating and the patient’s daily activity. Patients should be diagnosed early to get effective treatment and prevent dangerous complications.
You may find it useful to learn more about diagnostic measures of pericoronitis that are being applied today through this article.
What Causes Pericoronitis?
1. Accumulation of Bacteria
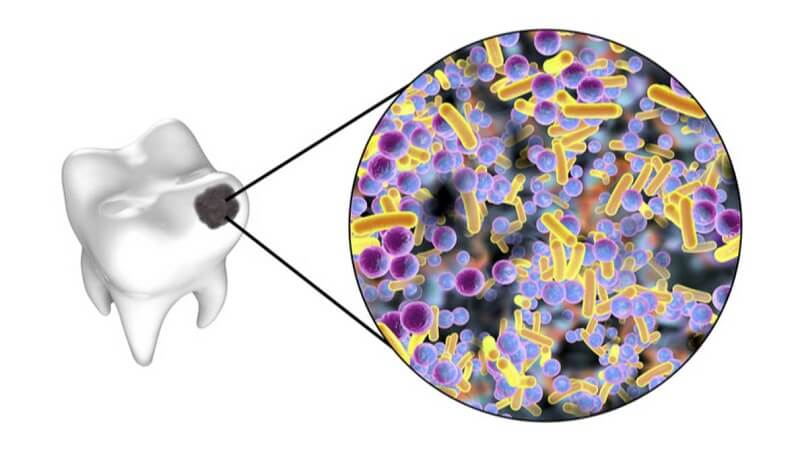
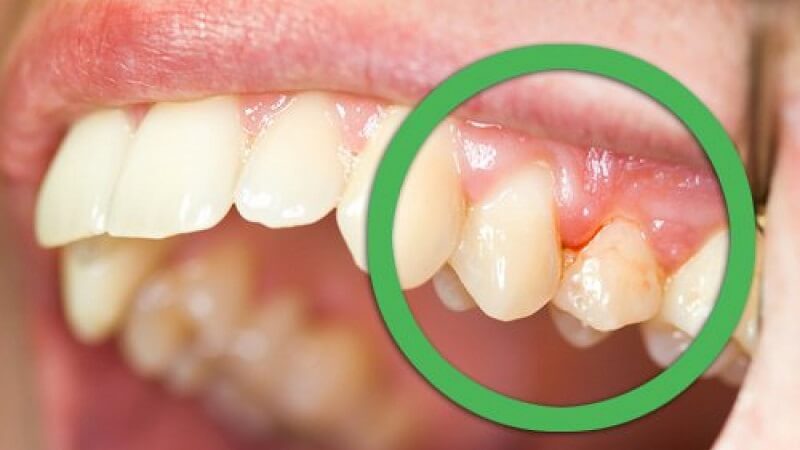
The primary cause of pericoronitis is the accumulation of bacteria. Usually, the tooth is only partially exposed (soft tissue impaction) and has excess gum tissue that overlaps the tooth. Bacteria and food debris get trapped in the space between the tooth and the overlapping gingiva. This overlapping gum flap is called an "operculum." Initially, inflammation of the operculum (operculate) takes place. A pericoronal infection can develop by the formation of an abscess under the operculum. If left unattended, the infection can spread to other soft tissue spaces.
2. Tooth Trauma
In the case of acute trauma: The trauma has a strong impact on the teeth, causing the blood vessels in the root of the tooth to rupture, which then creates favorable conditions for bacteria to easily penetrate, causing inflammation.
In the case of chronic trauma: The trauma is only mild, typically such as the auxiliary knob, the injury to the bite joint, the trauma caused by the habit of grinding teeth, and other bad habits such as nail-biting, thread biting, etc long-term repetition of chronic inflammatory lesions around the root canal.
3. Treatment Error
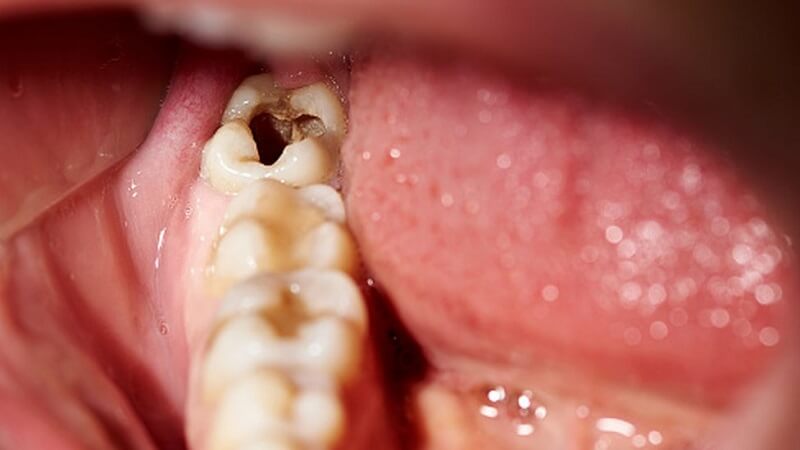
The cause of inflammation around the crown of the tooth can be due to excess fillings, taken too high leading to occlusion injury, or it can also be due to errors in the treatment of marrow for patients such as:
- Superinfection can occur during the extraction of the canal and the cleaning of the canal, pushing the dirt out of the stem area.
- The canal is blocked by mechanical factors, which may be tool breakage or organic factors such as the process of creating the dentin plug in the canal.
- During the marrow treatment, there is an infection but accidentally pushed into the stem area or foreign objects invade.
- Tearing wide or moving the stem hole.
- The use of antiseptics with strong doses or has strong stimulant properties affects the stalk area.
- The lost path leading to a punctured canal.
- The bacteria in the medullary cavity cause effects against antiseptic agents in the canal in the teeth during root canal treatment.
How Do You Diagnose Pericoronitis?
According to the International Classification of Diseases, pericoronitis can be classified as acute and chronic pericoronitis.
1. Acute Pericoronitis
Definitive Diagnosis
The doctor will rely on the clinical signs to diagnose acute pericoronitis as follows:
Systemic manifestations: The patient feels tired, has a high fever of over 38 C and develops typical signs of infection with a dirty tongue, dry lips, and a ganglion reaction occurring under the chin or area under the jaw.
Mechanical manifestations: Teeth aches appear with natural manifestations, there may be continuous pain with severity, the pain spread to the first half, when chewing the pain level will increase. This condition does not respond to pain relievers, the patient can determine the location of the toothache.
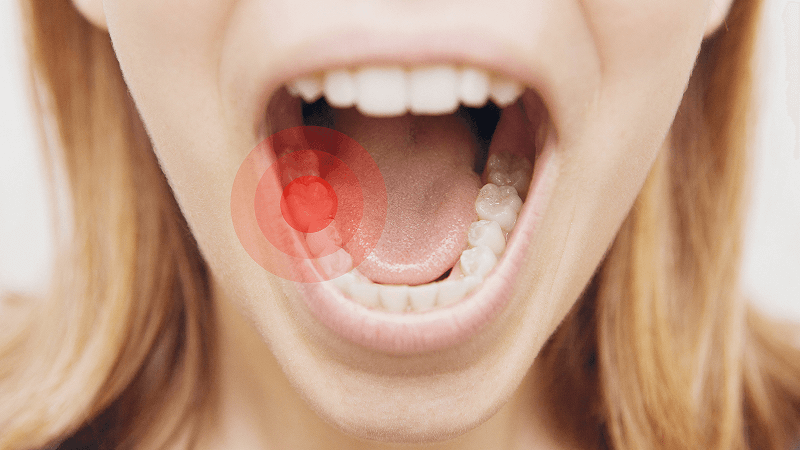
Besides, the patient with acute pericoronitis feels tooth protrusion, tooth pain when chewing, biting food, restricting eating.
Clinical Features: Corresponding to the location of the damaged tooth, usually the outer skin will be swollen, red, without a clear boundary, when pressed, there is pain and lymph nodes respectively. The affected tooth may or may not be discolored. On examination, the damage caused by the tooth decay is not yet welded, or the tooth has been treated or has other damage other than cavities.
Besides, it is possible to detect obvious signs of loose teeth, usually at level 2 – 3, when the doctor is knocking along the teeth, the patient will feel more intense pain than horizontal knocking.
At the same time, the mucous membrane of the gums is swollen and red, when pressed is painful, the tissue is loose. When conducting a test, the marrow will be negative for heat and electrical tests because the marrow is now necrotic.
In addition, valuable subclinical findings to help diagnose acute periosteal inflammatory disease include:
- X-ray: Through X-ray, you will observe an open image in the stem area, with unclear boundaries and accompanied by an enlarged ligament around the stem.
- Blood test: The result is that the rate of blood sedimentation increases, the number of neutrophils increases, etc.
Differential Diagnosis
Acute myelitis will have the following signs:
- No signs of a full body.
- Features of the pain: are natural pain, pain in bouts, often appear at night and pain will increase gradually when the patient chews food.
- When tapping along the teeth, there will be less pain, conducting a bone marrow test will give a positive result, through X-ray film with images of the stalk region will give normal results.
Acute Pericoronitis will have the following signs:
- Systemic signs: The patient has a feeling of fatigue, high fever, and regional lymphadenopathy.
- Characteristics of pain: Natural pain lasts smoldering, teeth appear loose and high buds.
- When tapping along the teeth, it will hurt less, but the marrow test is negative, X-ray film shows ligament enlargement.
2. Half Acute Pericoronitis
Definitive Diagnosis
Clinically, the patient's body condition will be diagnosed basing on the following signs:
Systemic manifestations: Patients have a feeling of discomfort, headache, mild fever, usually below 38 degrees, in some cases without fever.
Mechanical symptoms: The patient suffers from a dull pain in the damaged tooth, feels the tooth buds high, the pain will be more severe when the jaws touch each other.
The physical symptoms will include: the gum line corresponding to the affected tooth area is slightly swollen, red, and thickened, and when pressed, there is pain. However, it is common to experience less swelling in the respective outer skin, sometimes with a small, mobile nodule. The patient's teeth may or may not be discolored.
In addition, half acute pericoronitis will cause tooth decay damage occurring in the tooth surfaces, teeth being wobbly at level 1 – 2 when the doctor knocks along the patient will feel more pain with horizontal percussion. However, negative results were found through the marrow test.
For the subclinical side, through x-ray film can observe blurred images in the stalk region, and mild ligament relaxation in the peduncle area.
Differential Diagnosis
Acute pericoronitis has the following signs:
- Systemic signs: The patient has a feeling of fatigue, high fever, regional lymphadenopathy occurs.
- Characteristics of pain: is natural pain, lingering dullness, teeth manifesting high, loose buds.
- When typing along the teeth will feel a lot of pain.
For half acute pericoronitis has the following signs:
Systemic signs: The patient feels uncomfortable, has a fever over 38 degrees, or may not have a fever.
- Characteristics of pain: Patients with dull pain in damaged teeth, when two jaws touch each other, pain increases and teeth shoot high.
- When typing along will hurt a little.
3. Chronic Pericoronitis
Clinical signs to help your doctor identify chronic pericoronitis include:
Functional symptoms: The patient has only a history of toothache in acute myelitis episodes, acute periosteal inflammation, or acute periosteal abscess.
Physical symptoms: Teeth discoloration was observed that changed, turned opaque gray in the dentin, and had a sheen through the enamel.
The corresponding niche around the crown of the tooth may be slightly swollen, and a fistula or scarring in the base area. There are cases where the fistula does not appear in the socket but is on the skin, possibly in the base of the nose depending on the location of the abscess and cyst.
When the doctor knocks the teeth, the patient usually has no pain or only mild pain in the root area. In addition, teeth can become loose, which occurs when alveolar bone resorption occurs. The marrow test was negative.
Through x-ray film to examine subclinical manifestations, for pericoronitis, the doctor will notice:
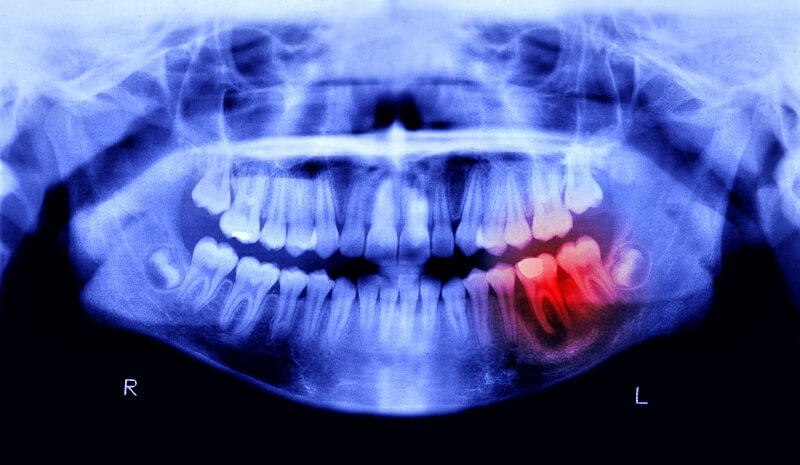
- Chronic peri-stem abscess: Shows bone resorption with no clear boundaries.
- When the doctor puts gutta-percha through the fistula in the patient's mouth, an image of the origin of the pus can be observed on X-ray imaging.
- Granulomas and cysts: Show bone resorption but differ from chronic peduncle abscess with clear boundaries.
Particularly in cases of chronic inflammation around the stalk, a biopsy must be performed to be able to accurately distinguish the disease.
After having confirmed the form of the disease, based on this result, the doctor will make decisions about the treatment of pericoronitis with the most suitable regimen for each case.
Hopefully, through this article, you will have a better understanding of inflammation around the root canal and current diagnostic testing methods.
We hope this article will be useful for you to learn more about pericoronitis and diagnose measures.
In order to control the disease well and have treatment regimens such as endodontic treatment, the whole body, surgery, patients need to identify signs and symptoms early to check – up and prevent complications that affect their health.
Please find the nearby location or the nearest branch your home to visit for tests and get quick online results. For more detailed information about our test menu and price list, visit here.
The site cannot and does not contain medical advice. The medical information is provided for general informational and educational purposes only and is not a substitute for professional advice. Accordingly, before taking any actions based upon such information, we encourage you to consult with the appropriate professionals.

 1900 1717
1900 1717 