According to statistics, fungal skin diseases are common diseases, accounting for about 27%. This is a pathology that can be passed from person to person with common ways such as fungal spores that spread through the air, or a sick person spread to a healthy person … the rest of the members are also at high risk of getting sick from sharing beds and sharing personal belongings with sick people.
Causes of Fungal Skin Infections
Fungal skin diseases are now becoming diseases with a high degree of popularity, the cause of this situation is first of all to the climate of Vietnam.
Because our country belongs to a hot and humid climate, in the tropics, it will be favorable conditions for fungal skin diseases to develop well. The most common types of fungal skin diseases are vitiligo, ringworm…
Fungi are inferior organisms because they do not have chlorophyll, so they cannot synthesize organic matter by themselves.
The host can be any typical source around us such as plants, animals (dogs, cats, buffaloes, cows …), and humans. Because of the high possibility of infection, it makes fungal skin diseases gradually becoming the most common skin diseases today.
In addition, unscientific living regimes, poor hygiene conditions are also favorable factors that cause fungal skin diseases to develop, typically:
- Skin fungus will proliferate and grow in an alkaline environment, with a pH in the range of 7 – 7.2.
- Bad personal hygiene is also the cause of the genital fungus.
- People with active sweat glands, places that produce a lot of sweat, especially between the hands and feet, and improper use of soap are also susceptible to fungal skin diseases.
- When the climate, the living environment is humid, people sweat a lot but wear cramped clothes, and the high temperature of about 27 – 35% is also a favorable factor for fungus to grow.
- The use of immunosuppressants or antibiotics, and women with endocrine disorders are at high risk of fungal infections.
Common Fungal Skin Diseases
Tinea Versicolor
Tinea versicolor caused by the agent is the fungus Pityrosporum, which is one of the common fungal skin diseases. The disease includes 2 forms: vitiligo black and white benign. A place with a warm and humid climate is a very favorable condition for fungus to grow.
The disease is common in young people who often have sweat glands, oily skin, people with immunodeficiency, pregnancy and are being treated with corticosteroids …
When infected, it will make the patient itchy, sometimes with an unpleasant stinging sensation. The disease often depends a lot on the problem of skin hygiene and the resistance of the patient. Therefore, there are cases, even though someone in the family has vitiligo, but other relatives do not get sick.
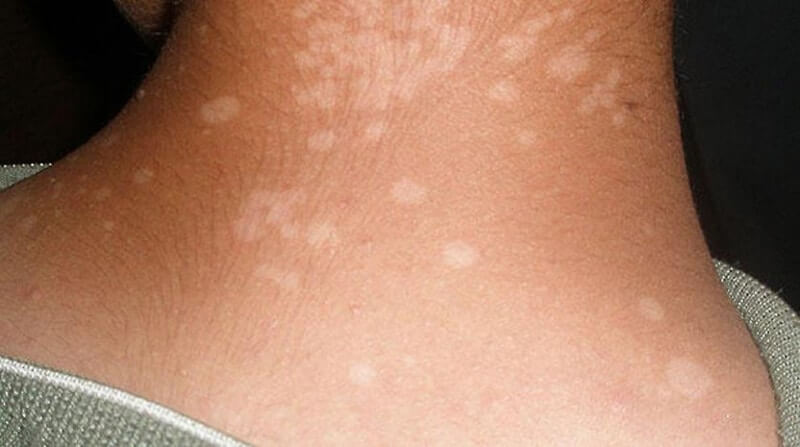
Vitiligo causes lesions on the skin that are oval or round, thinly scaly on the skin. You can try to see if you have leprosy by using your hand to gently scratch the surface of the lesion to detect a flake-off.
When there are widespread lesions, they will link together to form large plaques. Usually appears in the skin with seborrhea such as the chest, shoulder blades. In addition, it can cause damage to the face, breasts, and groin.
Ringworm
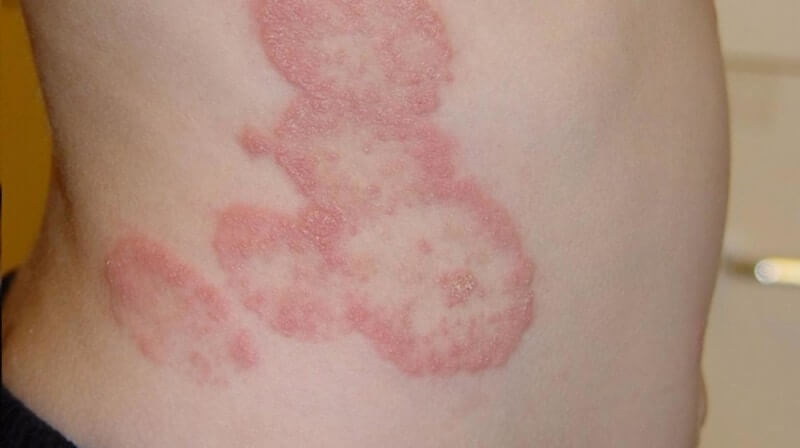
Ringworm is also one of the typical fungal skin diseases. When infected with ringworm, the first manifestation that the patient feels is the itchy area, then a reddish-colored streak will appear, with very noticeable edges and borders, and on the border, there will be Dotted blisters appear.
This mushroom border over time will tend to spread more and more and create more arcs. The disease causes an itchy, unpleasant sensation. When the patient scratches, the ringworm will continue to spread throughout the body.
The main cause of ringworm is a fungus that belongs to the Dermatophytes group. When sharing household utensils, sharing a bed, or sharing clothes with the sick person increases the risk of ringworm.
Athlete’s foot
Zinc is caused by the fungus Epidermophyton, trichophyton fungus or it can also be caused by the fungus Candida albicans. According to folklore also known by other names is water to eat feet of interstitial inflammation.
High-risk subjects that are susceptible to the disease are people who have to soak their feet frequently in water for a long time such as swimmers, farmers, sewer cleaning workers without careful protection … Interstitial fungus is divided into 3 main types: blister form, dry exfoliative and interstitial inflammation.
Nail fungus
Trichophyton is one of the main causes of onychomycosis. In particular, the mycelium (dermatophytes) accounts for a high proportion in cases of onychomycosis, usually over 90%.
Onychomycosis often appears on the free edge of the nail, which can also be 2 next to the nail, causing the inside of the nail to be damaged, and the nail that grows out will be deformed, erupted, the skin around the nail red swollen red if injured.
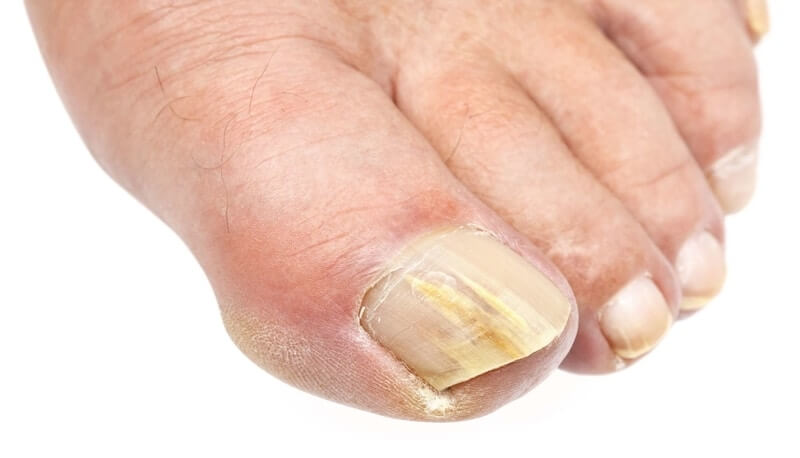
More severe cases of onychomycosis may develop pus, discolor the nail, become rough, or turn yellow or white. At the same time, the disease has the ability to spread from infected nails to healthy nails.
Besides the fungus trichophyton, which is the main cause of onychomycosis, there is also Candida albicans, which also damages the inside corners of the nail.
Trichomycosis
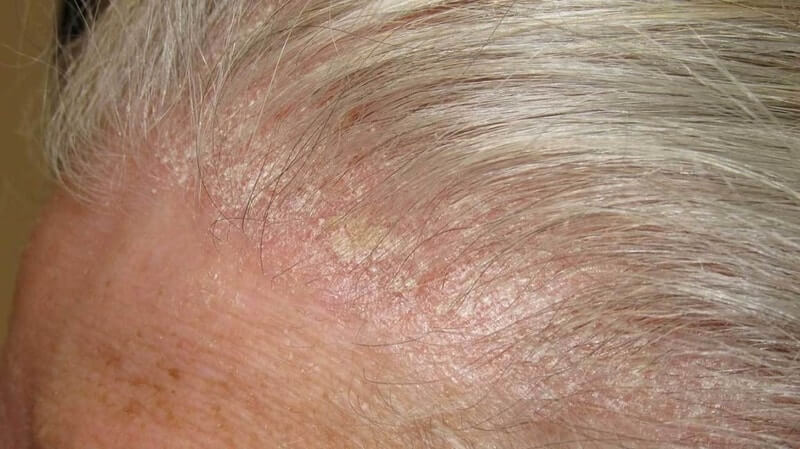
The main cause of hair fungus is the fungus dermatophyte is caused by fungus. In particular, scalp fungus caused by trichophyton will cause manifestations on the damaged skin area. At first, small nodules will appear scattered on the scalp.
If the disease is not treated at this stage, it will make the disease more serious, making more thin scaly patches appear. When these scabs are flaky, the scalp of the patient will be temporarily bald.
Pathogens such as Trichosporon Beigelii and Pierdraiahortai only develop in the hair shaft of the patient and do not cause hair loss.
The manifestation of this fungal hair disease is that on the hairline about 2 – 3 cm, there will be small, round, soft millet seeds.
The disease causes discomfort, often occurs with people who pay little attention to clean personal hygiene, the scalp is always wet, sweating …
Jock itch
The groin fungus is one of the common mycelia on the skin in people with poor hygienic awareness or immunocompromised, typically with diabetes, being overweight, obese, and wet genitals. Cleanliness…
When you have groin fungus, the first symptoms are red, sometimes brown, or gray in people with dark skin, accompanied by swelling and itching in the area. inguinal folds from the appearance of red skin gradually down to the groin, to the inside of the thighs and waist, buttocks.
At a later time, the damaged skin will be scaly and have a borderline higher than the healed area, which may be accompanied by flaking and cracking, causing increased pain and itching.
Treating Fungal Skin Disease
For some common fungal skin diseases, most of them are benign diseases, do not cause serious problems affecting the health of the patient. However, this is a contagious disease and affects the daily activities of the patient such as causing itching and discomfort.
When the disease is not treated early, it will make the disease last a long time, do not stop but recur many times and the next time will be worse than the last, making treatment more difficult.
Therefore, when you notice signs of suspicion of fungal diseases on the skin, you should consult a dermatologist for prompt diagnosis and treatment.
Where is mycosis examined? Currently, there are many hospitals and medical centers specializing in dermatological examinations. You should go to a reputable place to be accurately diagnosed with the condition such as:
- Central Dermatology Hospital – 15A Phuong Mai, Dong Da, Hanoi.
- Bach Mai Hospital – 78 Bach Mai, Dong Da, Hanoi.
- Ho Chi Minh City Dermatology Hospital – No. 2, Nguyen Thong, Ward 6, District 3, HCMC.
- The University of Medicine and Pharmacy Hospital – 215 Hong Bang, Ward 11, District 5, Ho Chi Minh City.
In addition, for online advice and answers to questions related to fungal skin diseases, you can also contact hotline 19001717 – Diag to get the fastest support.
Fungal skin diseases and treatment will have to depend on each specific case, at this time, the doctor can prescribe to the patient drugs applied directly to the damaged skin to treat mycelia skin diseases such as Clotrimazole Ciclopiroxolamin, Ketoconazole …
Patients should pay attention to use drugs according to the instructions of the doctor and follow-up periodically, if any, to monitor the condition of the disease and to adjust accordingly.
In addition, to quickly improve the disease, some living habits also need to be changed to limit more serious fungal inflammation such as:
- Pay attention to clean personal hygiene, wear clean, cool clothes, wear well-ventilated slippers, and limit barefoot in public places such as changing rooms, gyms. Avoid wearing shoes if you have foot fungus.
- Wash soapy-clean clothes and dry them in the hot sun to kill bacteria or regular clothes, especially underwear.
- Avoid contact with sources of animal diseases.
- Absolutely do not share personal belongings with someone who is sick.
Avoid using products that contain a lot of chemicals for cleaning such as detergents and soaps during the healing period. Take a bath with clean water only and choose benign products. Appropriate products can be consulted by a doctor.

- Should regularly clean for a clean living space.
Hopefully, this article has provided you with useful information related to the common fungal skin diseases today. Because the disease is contagious, care should be taken to keep the disease clean to limit the risk of disease. As soon as there are suspicious symptoms, you should go to the hospital for diagnosis and treatment to prevent the disease from spreading to the healed areas to prolong the recovery time.
For more information about our test menu and price list, please click here.
The site cannot and does not contain medical advice. The medical information is provided for general informational and educational purposes only and is not a substitute for professional advice. Accordingly, before taking any actions based upon such information. We encourage you to consult with the appropriate professionals.

 1900 1717
1900 1717 